Use of the frenectomy procedure in periodontics (unlike in orthodontic or pediatric applications) is limited because of the minimal increase in attached gingiva observed after postfrenectomy wound healing (Figure 4-6). Alveolar mucosa is characterized by a red color and a smooth surface and generally is loose and mobile, whereas attached gingiva is keratinized, pink, stippled, and firm, with no mobility (Figure 4-7).
Gingival surgery in the form of soft tissue augmentation is necessary under the following conditions:
• Marginal gingiva is inflamed.
• Bleeding or exudate is present at the sulcus/pocket.
• Obvious recession is present.
• Pulling of marginal tissue occurs with retraction of the lip.
• As determined by direct measurement, the sulcular depth in millimeters is subtracted from the keratinized zone of gingiva. At least 2 mm of “keratinized attached gingiva” should be present.
Frenectomy procedures with a laser are predictably successful so long as the following steps are incorporated:
1. Creation of a periosteal fenestration at the base of the frenectomy to prevent reattachment of fibers
2. Removal of all impeding muscle fibers
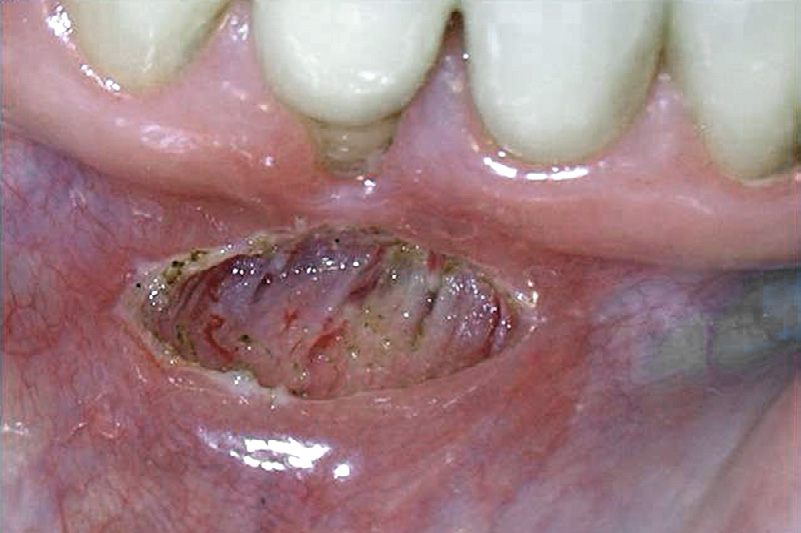
Figure 4-6 Immediate postoperative view of laser frenectomy site in a patient in whom the frenectomy was performed without consideration for the extent of gingival attachment, which was minimal to none. A mucogingival graft procedure or vestibuloplasty is indicated to gain an adequate amount of keratinized attached gingiva. Note hemostasis.
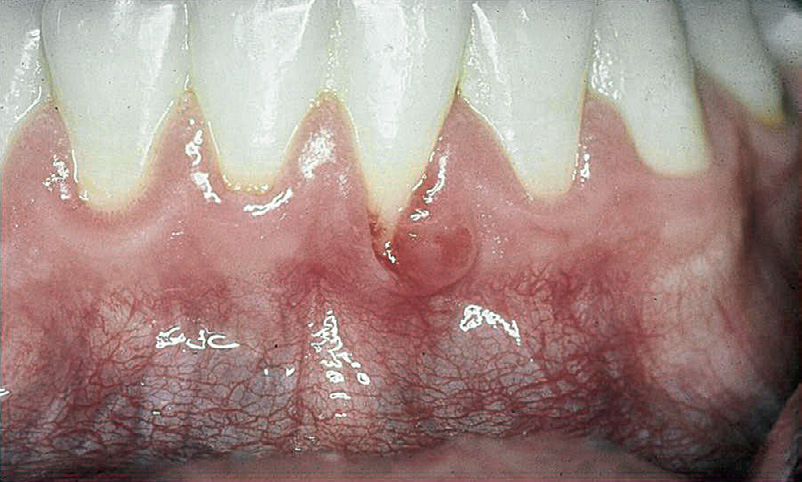
Figure 4-7 Comparison of alveolar mucosa and gingiva. Parameters of color, surface, and mobility are used in differentiating mucosa from gingiva. Mandibular left lateral incisor has a cleft that borders on alveolar mucosa. The level of inflammation makes discerning the level of attached gingiva difficult; this determination is best delayed until after health is achieved.
Parameter Alveolar Mucosa Gingivae
Color Red Coral pink
Surface Smooth Stippled
Mobility Loose Firm
All laser wavelengths can be used to perform a frenectomy successfully; however, depth of penetration for diode is much higher than for erbium or CO2 lasers, so settings must be monitored closely to prevent thermal damage to the underlying periosteum and bone. In some patients, topical anesthesia is sufficient to allow performance of a frenectomy, with excellent precision, and with less discomfort and shorter healing time than with conventional techniques. CO2 laser treatment for frenectomy provides better postoperative patient perceptions of control of pain and improved function than with the scalpel technique. Likewise, use of the Nd:YAG laser may result in less postoperative pain and fewer functional complications.
The technique for a laser frenectomy is similar to that using a blade (Figure 4-8). Local or topical anesthesia is administered. The clinician should first visualize the procedure by forming a mental outline of the incision. This incision begins at the coronal attachment; the laser tip is then moved unidirectionally, with tension achieved by pulling on the lip. With use of the correct parameters (spot size, power, hand speed), one pass of the laser should be sufficient to sever all of the fibers. If multiple passes are necessary, care must be taken to avoid excessive lateral thermal necrosis from reexposure of already-treated tissue. The laser incision is continued to undermine the muscle attachment until the periosteum is reached.
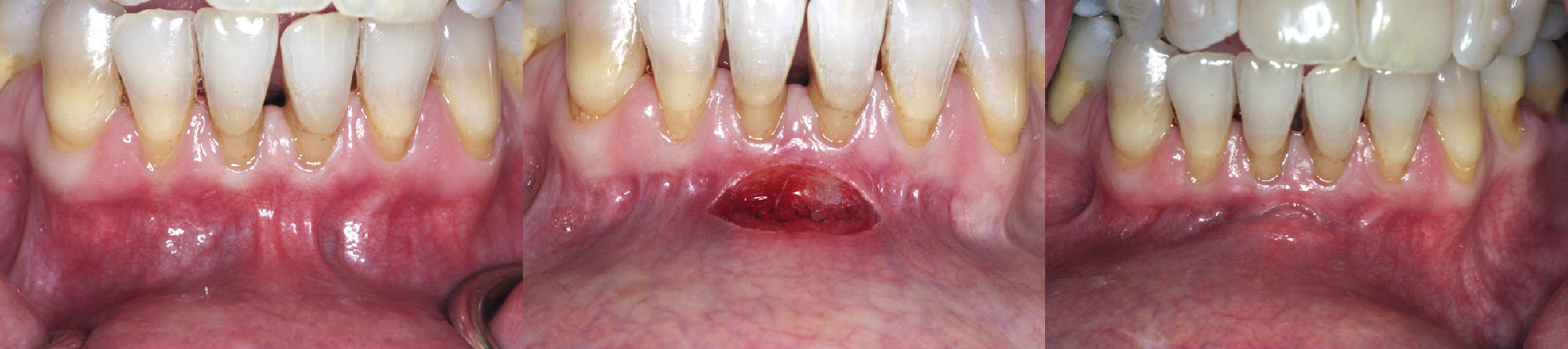
Figure 4-8 A, Preoperative view of frenum pull. B, Immediate postoperative view of laser frenectomy site. C, Postoperative view at 1 week. Note rapid healing.
To ensure minimal regrowth and prevent frenum“relapse”the periosteum should be fenestrated with a hand instrument. All lasers are effective for a frenectomy with settings suggested by the manufacturer. Care must be taken not to char the tissue, with consequent thermal tissue damage.
Clinical Tip
The greater the amount of tension placed on the frenum achieved by pulling on the lip, the faster the frenectomy proceeds.