A crown-lengthening procedure is used to gain access to subgingival caries, expose margins, and explore fractures. The procedure allows for developing a proper form for a restoration and increasing surface area for retention. The patient’s smile can be enhanced by manipulation of the gingival contour. When considering a crown-lengthening procedure, the clinician must address the following questions:
• Can biologic width be maintained?
• Will attached gingiva be preserved?
• Can opening and invading furcations be avoided?
• Is the tooth restorable?
• Will there be loss of support to the adjacent tooth?
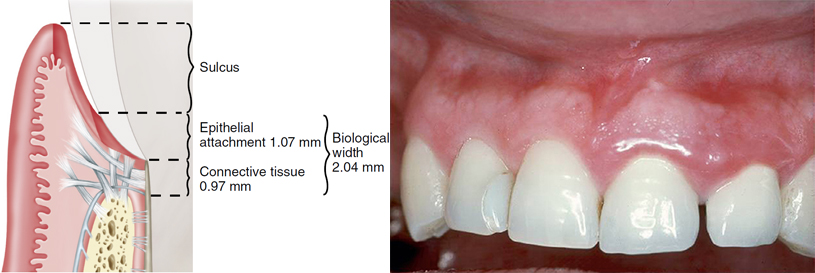
Biologic width. A, Diagram of relevant anatomy. B, Violation of biologic width with resulting inflammation. Standard measurement for biologic width is 2 mm; this includes epithelial and connective tissue attachment. When a restoration is placed into this zone and within 2 mm of the osseous level, a foreign body reaction occurs, resulting in inflammation.
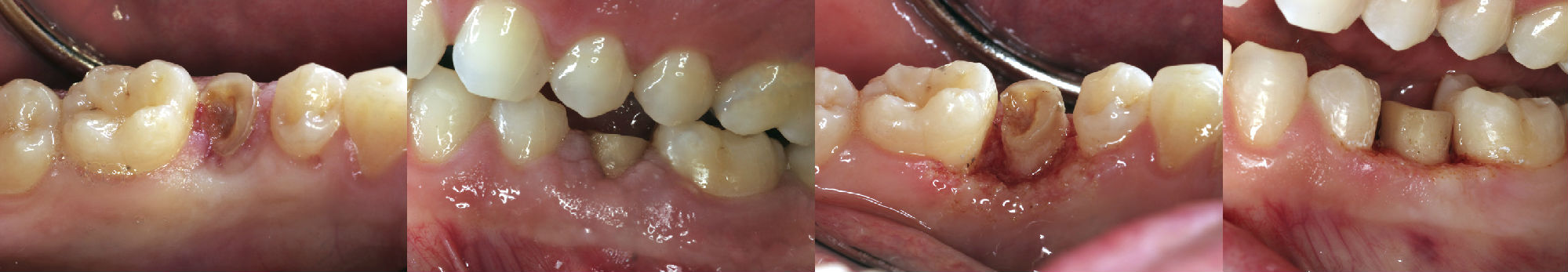
Closed-flap crown lengthening with laser (to achieve ostectomy). Preoperative views: lingual (A) and buccal (B). Immediate postoperative views: lingual (C) and buccal (D). The patient presented with a coronal fracture of questionable prognosis. Sounding bone levels determined that osseous levels would require apical alteration to achieve biologic width.
Contraindications to crown lengthening include attempting to retain a nonrestorable tooth, compromising adjacent teeth, compromised crown/root ratios, root proximity issues, and unrealistic expense. The technique of laser crowning lengthening varies with the laser type. If the objective is soft tissue, the diode laser is sufficient. However, to alter underlying osseous structures, erbium lasers and possibly the 9300-nm CO2 laser are used.
The following protocol establishes the necessary biologic width with due consideration of patient esthetics:
1. “Sound” the osseous crest (3.0 mm from osseous crest to proposed gingival margin).
2. Provide zone of keratinized gingival margin (scallop desired lengths if 3 mm or more will be retained).
3. Bevel papillary areas (levels can be apically positioned and adjusted later).
4. Leave papilla intact at base.
5. Thin the osseous crest, but leave at least 1 mm of thickness.
6. Determine whether dentin/root surfaces will be exposed (plan treatment for restorative procedures).
In laser crown-lengthening techniques, first determine the apical extent of the presumed restorative margin. If it is determined that the margin will be within 2 to 3 mm of the osseous crest, osseous surgery inevitably will be required to maintain the biologic width. Therefore a flap reflection will be necessary, or a “closed” flap crown-lengthening procedure must be considered.
Controversy surrounds the closed-flap crown-lengthening procedure when bone is removed. This surgery can be challenging because it involves “blind” sounding of the osseous levels, and removal of bone can be unpredictable. If no osseous surgery is required, and if the end result will maintain adequate attached gingiva, a modified laser gingivectomy procedure will provide the necessary access for crown length, especially in the anterior esthetic zone.
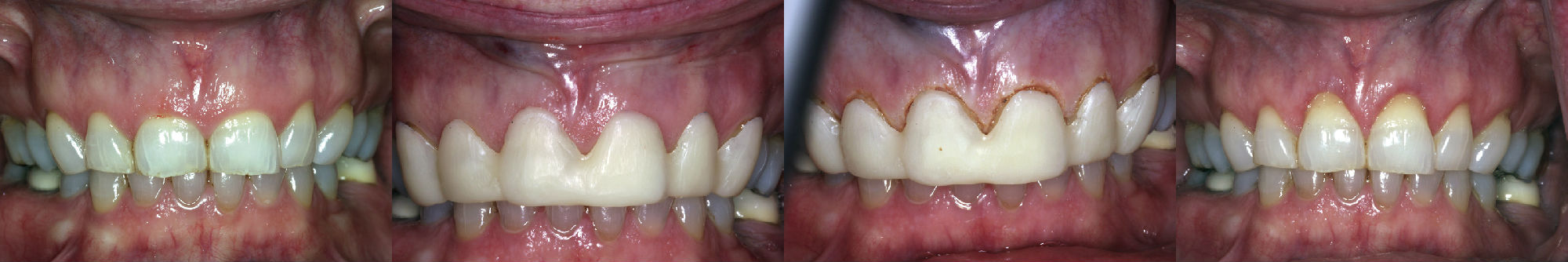
Laser crown-lengthening procedure for restoration of maxillary and mandibular anterior teeth. A, Preoperative view. B, C, Closed-flap crown-lengthening approach was used, with creation of a surgical stent. The erbium wavelength was chosen for the required osseous surgery. Note minimal hemorrhage. D, Two-week postoperative view.
To begin an esthetic crown-lengthening procedure, the clinician may want to fabricate a surgical guide or stent to assist in determining the apical extent of the gingival margin, using the principles of ideal width and height of respective tooth types. After local anesthesia is obtained with infiltration, the following steps can be performed with most dental lasers when osseous surgery is not necessary:
1. With the surgical guide in place, an outline of the initial incision can be made with the laser in a slightly defocused mode. As with a conventional blade-initiated gingivectomy, the laser incision is started slightly apical to the stent and at a 45-degree angle to create a gingival chamfer.
2. The stent can be removed after the outline, and with the laser tip moving slowly in a unidirectional manner, the tip is increasingly moved toward the tooth surface. Caution is necessary for preserving the papillae for esthetics.
3. The now-free excised collar can be removed with a curette and the stent replaced to check the accuracy of margin placement.
4. With a relatively lower wattage, the laser tip can now be moved in a sweeping motion to sculpt the margin and enhance the chamfer and to decrease gingival thickness to a more knifelike architecture. Placement of the laser subgingivally is not necessary unless osseous surgery is needed and the erbium laser is required to establish the biologic width.
5. The resulting wound will exhibit minimal hemorrhage. Again, the laser bandage technique is used at the clinician’s discretion.
6. Postoperative care consists of gentle brushing and antimicrobial rinsing for 2 weeks. Whether or not to place a surgical dressing is again the clinician’s decision. After 2 weeks, patients return to conventional oral hygiene, with a soft brush for sulcular cleaning and flossing for interproximal hygiene.
Rather than using a stent, some lasers can be used in an intermittent exposure mode (not to be confused with pulsed delivery). This intermittent delivery allows the surgeon to outline margins of a gingivectomy before performing an irreversible incision. This technique is routinely used in other disciplines of dentistry, especially in outlining margins of a planned biopsy specimen.